Darvon, Darvocet Banned
Controversial Painkiller Sunk by Dangerous Heart Side Effects
Reviewed by Louise Chang, MD
Nov. 19, 2010 -- The FDA has at last banned Darvon, Darvocet, and other brand/generic drugs containing propoxyphene -- a safety-plagued painkiller from the 1950s.
New proof of heart side effects, in studies of healthy people taking normal doses of the drug, prompted the FDA to act.
An estimated 10 million Americans are taking Darvocet and other propoxyphene painkillers. They should NOT immediately stop taking the drugs, as there is danger of serious withdrawal symptoms.
Patients taking the drugs should instead immediately contact their doctors for help switching to different methods of pain control.
"Don't delay," warns Gerald Dal Pan, MD, MHS, director of the FDA's office of surveillance and epidemiology.
The FDA action comes nearly six years after the drug was banned in the U.K., and nearly a year and a half after the European drug agency banned it.
The public interest group Public Citizen petitioned the FDA to ban the drug in 1978 and again in 2006. The latter petition caused the FDA to take the matter to an expert advisory committee, which in July 2009voted 14-12 to ban the drug.
But the FDA overruled the panel, instead asking Darvon/Darvocet maker Xanodyne Pharmaceuticals Inc. to conduct studies of the drug's effects on the heart. The results of those studies led to the FDA ban.
"The drug puts patients at risk of abnormal or even fatal heart rhythm abnormalities," John Jenkins, MD, director of the FDA's office of new drugs at the Center for Drug Evaluation and Research, said at a news conference. "Combined with prior safety data, this altered our risk assessment."
The FDA ban comes too late for Public Citizen, which blasted the FDA for waiting far too long to protect the public.
"Due to FDA negligence, at least 1,000 to 2,000 or more people in the U.S. have died from using propoxyphene since the time the U.K. ban was announced," Sidney Wolfe, director of Public Citizen's health research group, says in a news release.
Wolfe says Public Citizen will call for a congressional investigation into who at the FDA "was responsible for the loss of so many lives in this country."
continued...
Jenkins says although it's impossible to know exactly how many deaths are linked to propoxyphene, an FDA study shows that more deaths are linked to the drug than to either of two alternative opioid painkillers,tramadol and hydrocodone.
Dal Pan says that people who have taken Darvocet, Darvon, or other propoxyphene drugs for a long time are not at increased risk of heart problems.
"Long-term users should not worry: The heart effects are not cumulative," he says. "Once people stop using propoxyphene, the side effects should go away."
More information about the propoxyphene ban is available on the FDA web site -- including, for the first time, a video news release.
© 2010 WebMD, LLC. All rights reserved.
From Wikipedia, the free encyclopedia
"Paradex" redirects here. For the antiseptic trade named Peridex, see Chlorhexidine. For the oral anticoagulant trade named Pradaxa, see Dabigatran.
"PPX" redirects here. For the online virtual prediction market, see Popular Science Predictions Exchange.
 | |
 | |
| Systematic (IUPAC) name | |
|---|---|
(1S,2R)-1-benzyl-3-(dimethylamino)-2-methyl-1-phenylpropyl propionate
| |
| Clinical data | |
| Trade names | Darvon |
| AHFS/Drugs.com | monograph |
| MedlinePlus | a682325 |
| Licence data | US FDA:link |
| Pregnancy category |
|
| Legal status |
|
| Routes of administration | oral, IV, rectal |
| Pharmacokinetic data | |
| Bioavailability | 40%[1] |
| Protein binding | 78%[1] |
| Metabolism | Liver-mediated, CYP3A4-mediated N-demethylation (major), aromatic hydroxylation (minor) and ester hydrolysis (minor)[1] |
| Biological half-life | 6–12 hours; 30–36 hours (active metabolite, nordextropropoxyphene)[2] |
| Excretion | Urine (major), breastmilk (minor)[1] |
| Identifiers | |
| CAS Registry Number | 469-62-5 |
| ATC code | N02AC04 |
| PubChem | CID: 10100 |
| IUPHAR/BPS | 7593 |
| DrugBank | DB00647 |
| ChemSpider | 9696 |
| UNII | S2F83W92TK |
| KEGG | D07809 |
| ChEBI | CHEBI:51173 |
| ChEMBL | CHEMBL1213351 |
| Chemical data | |
| Formula | C22H29NO2 |
| Molecular mass | 339.471 g/mol |
| Physical data | |
| Melting point | 75 °C (167 °F) |
| | |
Dextropropoxyphene[3] is an analgesic in the opioid category, patented in 1955[4] and manufactured by Eli Lilly and Company. It is an optical isomer of levopropoxyphene. It is intended to treat mild pain and also has antitussive (cough suppressant) and local anaesthetic effects. The drug has been taken off the market in Europe and the US due to concerns of fatal overdoses and heart arrhythmias.[5] Its onset of analgesia (pain relief) is said to be 20–30 minutes and peak effects are seen about 1.5–2 hours after oral administration.[1]
Dextropropoxyphene is sometimes combined with acetaminophen or aspirin. Trade names include Darvocet-N and Di-Gesic,[6] Darvon with APAP (for dextropropoxyphene and paracetamol) and Darvon with ASA (for dextropropoxyphene andaspirin).[7] The British approved name (i.e. the generic name of the active ingredient) of the paracetamol/dextropropoxyphene preparation is "co-proxamol" (sold under a variety of brand names); however, it has been withdrawn since 2007, and is no longer available to new patients, with exceptions.[8] The paracetamol combination(s) are known as Capadex or Di-Gesic in Australia, Lentogesic in South Africa, and Di-Antalvic in France (unlike co-proxamol, which is an approved name, these are all brand names).
Dextropropoxyphene is known under several synonyms, including:
- Alpha-d-4-dimethylamino-3-methyl-1,2-diphenyl-2-butanol propionate
- [(2S,3S)-4-(Dimethylamino)-3- methyl-1,2-diphenylbutan-2-yl] propanoate
- (+)-1,2-Diphenyl-2-propionoxy- 3-methyl-4-di-methylaminobutane
- Desoxypropiophen
Contents
[hide]
Uses[edit]
Analgesia[edit]
Dextropropoxyphene, like codeine, is a weak opioid, known to cause dependency among recreational users. Codeine is more commonly used; however, as codeine is, in essence, a prodrug that requires in vivo metabolism for efficacy, it is ineffective for some individuals with the "poor metabolizer" genotype of the liver cytochrome P450 enzyme CYP2D6. In people with this low-function isoform, dextropropoxyphene is particularly useful, as its metabolism does not require CYP2D6. It is also used for patients with digestive complaints, as it is less liable to worsen their symptoms.
Restless legs syndrome[edit]
Dextropropoxyphene has been found to be helpful in relieving the symptoms of restless legs syndrome.[9][10][11]
Opioid withdrawal[edit]
In pure form, dextropropoxyphene is commonly used to ease the withdrawal symptoms in people addicted to opioids. Being very weak in comparison to commonly abused opioids, dextropropoxyphene can only act as a "partial" substitute. It does not have much effect on mental cravings; however, it can be effective in alleviating physical withdrawal effects, such as muscle cramps.
Contraindications[edit]
Dextropropoxyphene is contraindicated in patients allergic to paracetamol (acetaminophen) or dextropropoxyphene, in alcoholics, and in combination with amphetamine, where CNS stimulation is potentiated and fatal convulsions can occur in dextropropoxyphene overdosage.[12] Dextropropoxyphene is not intended for use in patients who are prone to suicide, anxiety, panic, or addiction.
Side effects[edit]
| This section does not cite any references or sources. (November 2010) |
- Constipation
- Itching
- Drowsiness
- Sore throat
- Impaired alertness
- Confusion
- Serious or fatal heart rhythms
Pharmacology[edit]
Dextropropoxyphene acts as a mu-opioid receptor agonist. It also acts as a potent, noncompetitive α3β4 neuronal nicotinic acetylcholine receptor antagonist,[13] as well as a weak serotonin reuptake inhibitor.
Toxicity[edit]
Overdose is commonly broken into two categories: liver toxicity (from paracetamol poisoning) and dextropropoxyphene overdose.
An overdose of dextropropoxyphene may lead to various systemic effects. Excessive opioid receptor stimulation is responsible for the CNS depression, respiratory depression, aspiration pneumonia, miosis, and gastrointestinal effects seen in propoxyphene poisoning. It may also account for mood- or thought-altering effects.
In addition, both propoxyphene and its metabolite norpropoxyphene have local anesthetic effects at concentrations about 10 times those necessary for opioid effects. Norpropoxyphene is a more potent local anesthetic than propoxyphene, and they are both more potent thanlidocaine.[14] Local anesthetic activity appears to be responsible for the arrhythmias and cardiovascular depression seen in propoxyphene poisoning.[15]
Both propoxyphene and norpropoxyphene are potent blockers of cardiac membrane sodium channels and are more potent than lidocaine,quinidine, and procainamide in this respect.[16] As a result, propoxyphene and norpropoxyphene appear to have the characteristics of aVaughn-Williams Class Ic antiarrhythmic.
These direct cardiac effects include decreased heart rate (i.e. cardiovascular depression), decreased contractility, and decreased electrical conductivity (i.e., increased PR, AH, HV, and QRS intervals). These effects appear to be due to their local anesthetic activity and are not reversed by naloxone.[14][15][17] Widening of the QRS complex appears to be a result of a quinidine-like effect of propoxyphene, and sodium bicarbonate therapy appears to have a positive direct effect on the QRS dysrhythmia.[18]
Seizures may result from either opioid or local anesthetic effects.[14] Pulmonary edema may result from direct pulmonary toxicity,neurogenic/anoxic effects, or cardiovascular depression.[15]
Balance disorder is possible, with risk of falls from standing height.
Available forms[edit]
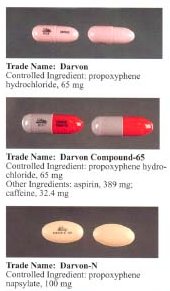
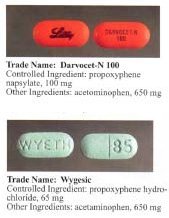
Propoxyphene was initially introduced as propoxyphene hydrochloride. Shortly before the patent on propoxyphene expired, propoxyphene napsylate form was introduced to the market. Napsylate salt (the salt of naphthalenesulfonic acid) is claimed to be less prone to abuse, because it is almost insoluble in water, so cannot be used for injection. Napsylate also gives lower peak blood level.[19] Because of different molecular mass, a dose of 100 mg of propoxyphene napsylate is required to supply an amount of propoxyphene equivalent to that present in 65 mg of propoxyphene hydrochloride.
Before the FDA-directed recall, dextropropoxyphene HCl was available in the United States as a prescription formulation with paracetamol (acetaminophen) in ratio from 30 mg / 600 mg to 100 mg / 650 mg (or 100 mg / 325 mg in the case of Balacet), respectively. These are usually named Darvocet. Darvon is a pure propoxyphene preparation that does not contain paracetamol.
In Australia, dextropropoxyphene is available on prescription, both as a combined product (32.5 mg dextropropoxyphene per 325 mg paracetamol branded as Di-gesic, Capadex, or Paradex; it is also available in pure form (100 mg capsules) known as Doloxene.
Drug testing[edit]
| This section does not cite any references or sources. (November 2010) |
Detectable levels of propoxyphene/dextropropoxyphene may stay in a person's system for up to 9 days after last dose and can be tested for specifically in nonstandard urinalysis, but may remain in the body longer in minuscule amounts. Propoxyphene will not show up on standard opiate/opioid tests because it is not chemically related to opiates as part of the OPI or OPI 2000 panels, which detect morphine and related compounds. It is most closely related to methadone.
Usage controversy and regulation[edit]
Dextropropoxyphene is subject to some controversy: while many physicians prescribe it for a wide range of mildly to moderately painful symptoms, as well as for treatment of diarrhea, many others refuse to prescribe it, citing limited effectiveness. In addition, thetherapeutic index of dextroproxyphene is relatively narrow.
Caution should be used when administering dextropropoxyphene, particularly with children and the elderly and with patients who may be pregnant or breast feeding; other reported problems include kidney, liver or respiratory disorders, and prolonged use. Attention should be paid to concomitant use with tranquillizers, antidepressants or excess alcohol.
Darvon, a dextropropxyphene formulation made by Eli Lilly, which had been on the market for 25 years, came under heavy fire in 1978 by consumer groups that said it was associated with suicide. Darvon was never withdrawn from the market, but Lilly has waged a sweeping, and largely successful, campaign[citation needed] among doctors, pharmacists and Darvon users to defend the drug as safe when it is used in proper doses and not mixed with alcohol. On November 19, 2010, the FDA banned all sale of Darvon and Darvocet.[20]
Australia[edit]
In Australia, both pure dextropropoxyphene capsules (as napsylate, 100 mg), marketed as Doloxene, and combination tablets and capsules (with paracetamol) all containing 32.5 mg dextropropoxyphene HCl with 325 mg paracetamol, which are currently available on prescription were supposed to be withdrawn from 1 March 2012,[21] but Aspen Pharma sought a review in the Administrative Appeals Tribunal which resulted in a stay in the ban until a hearing scheduled for late May.[22] In 2013 the Administrative Appeals Tribunal ruled that the drugs could be sold under strict conditions.
European Union[edit]
In November 2007, the European Commission requested the European Medicines Agency (EMA) to review the safety and effectiveness of dextropropoxyphene based medicines and on 25 June 2009 the EMA recommended a gradual withdrawal throughout the European Union. The EMA's conclusion was based on evidence that dextropropoxyphene-containing medicines were weak painkillers, the combination of dextropropoxyphene and paracetamol was no more effective than paracetamol on its own, and the difference between the dose needed for treatment and a harmful dose (the "therapeutic index") was too small.[23]
New Zealand[edit]
Sweden[edit]
In Sweden, physicians had long been discouraged by the medical products agency to prescribe dextropropoxyphene due to the risk of respiratory depression and even death when taken with alcohol.[25] Physicians have earlier been recommended to prescribe products with only dextropropoxyphene and not to patients with a history of drug abuse, depression or suicidal tendencies. Products with mixed active ingredients were taken off the market and only products with dextropropoxyphene were allowed to be sold. Dextropoxyphene was de facto narcotica labelled. As of March 2011, all products containing the substance are withdrawn because of safety issues after a European Commission decision.[26][27]
It was discussed at the time that people who abuse alcohol and other substances and take combination dextropoxyphene / acetaminophen (paracetamol) may need to take many combination tablets to reach euphoria, because the amount of dextropropoxyphene per tablet is relatively low (30–40 mg). The ingested paracetamol - the other component - may then reach liver toxic levels. In the case of alcoholics, who often already have damaged livers, even a relatively small overdose with paracetamol may produce hepatotoxicity, liver necrosis and liver failure. This toxicity with the combination of overdosed dextroproxyphene (with its CNS/respiratory depression/vomit with risk foraspiration pneumonia, as well as cardiotoxicity) and paracetamol-induced liver damage can result in death.
United Kingdom[edit]
In the United Kingdom, preparations containing only dextropropoxyphene were discontinued in 2004.[28] In 2007, the Medicines and Healthcare Products Regulatory Agencyremoved the licence for co-proxamol, also called distalgesic.[29] From then on in the UK, co-proxamol is only available on a named patient basis, for long-term chronic pain and only to those who have already been prescribed this medicine. Its withdrawal from the UK market is a result of concerns relating to its toxicity in overdose (even small overdoses can be fatal), and dangerous reaction with alcohol. Recreational use in the UK is uncommon. Many patients have been prescribed alternative combinations of drugs as a replacement.[30]
The motivation for the withdrawal of co-proxamol was the reduction in suicides and a key part of the agency's justification of its decision was based upon studies showing co-proxamol was no more effective than paracetamol alone in pain management.[31] Prescribing authorities, such as the Royal College of General Practitioners, unanimously recommended withdrawal, while patients who responded to the agency's request for information tended to want to continue treatment.[32]
The co-proxamol preparations available in the UK contained a subtherapeutic dose of paracetamol, 325 mg per tablet.[33] Patients were warned not to take more than eight tablets in one day, a total dose of 2600 mg paracetamol per day. Despite this reduced level, patients were still at a high risk of overdose; coproxamol was second only totricyclic antidepressants as the most common prescription drugs used in overdose.[31] Following the reduction in prescribing in 2005–2007, prior to its complete withdrawal, the number of deaths associated with the drug dropped significantly. Additionally, patients have not substituted other drugs as a method of overdose.[34]
The decision to withdraw coproxamol has met with some controversy; it has been brought up in the House of Commons on two occasions, 13 July 2005[35] and on 17 January 2007.[36] Patients have found alternatives to co-proxamol either too strong, too weak, or with intolerable side effects.[citation needed] During the House of Commons debates, it is quoted that originally some 1,700,000 patients in the UK were prescribed co-proxamol. Following the phased withdrawal, this has eventually been reduced to 70,000. However, it appears this is the residual pool of patients who cannot find alternate analgesia to co-proxamol.[citation needed]
The safety net of prescribing co-proxamol after license withdrawal from 31 December 2007, on a "named patient" basis where doctors agree there is a clinical need, has been rejected by most UK doctors[citation needed] because the wording that "responsibility will fall on the prescriber" is unacceptable to most doctors. Some patients intend to take the case to the European Court of Human Rights.[37] However, the European Medicines Agency has recently backed the agency's decision, and recommended in June 2009 that propoxyphene preparations be withdrawn across the European Union.[38]
United States[edit]
In January 2009, an FDA advisory committee voted 14 to 12 against the continued marketing of propoxyphene products, based on its weak pain-killing abilities, addictiveness, association with drug deaths and possible heart problems, including arrhythmia. A subsequent re-evaluation resulted in a July 2009 recommendation to strengthen the boxed warning for propoxyphene to reflect the risk of overdose.[39] Dextropropoxyphene subsequently carried a black box warning in the U.S., stating:
Because of potential for side effects, this drug is on the list for High Risk Medications in the elderly.[41]
On November 19, 2010, the FDA requested the cessation of all sale of Darvon and Darvocet from the US drug market due to heart arrhythmia in patients who took the drug.[42] The drug Darvocet may also be involved in combined drug intoxication, because it may lead to confusion in patients and physicians. Many doctors are commonly switching to tramadol, because it is more effective than Darvocet yet is believed to be less addictive than stronger hydrocodone based medications.[citation needed] However, in the same way codeine is a prodrug that requires in vivo metabolism for efficacy, tramadol is as well. So in the same manner as codeine, tramadol can be ineffective for individuals with liver enzyme CYP2D6 deficiencies. This can sometimes make propoxyphene a "last resort" for minor pain relief in people with this condition, as even much stronger opioids such as hydrocodone and oxycodone will also be slightly less effective as much as 10% of these medications will be converted to the much strongerhydromorphone and oxymorphone, respectively, in typical patients. In these cases medications like morphine or tapentadol can be used as they do not require further metabolism to be effective. However, these medications are many times stronger than propoxyphene, and come with their own set of risks, including a much larger risk of overdose and addiction than propoxyphene.
Bulk dextropropoxyphene is a Schedule II controlled substance with a DEA ACSCN of 9273 and a 2013 annual aggregate manufacturing quota of 19 grammes.
Canada[edit]
On December 1, 2010, Health Canada and Paladin Labs Inc. announced the voluntary recall and withdrawal of Darvon-N from the Canadian market and the discontinuation of sale of Darvon-N.[43]
India[edit]
On June 12, 2013, the Indian government suspended the manufacture, sale, and distribution of the drug under Section 26A of the 1940 Drugs and Cosmetic Act.[44]
Use by right to die societies[edit]
High toxicity and relatively easy availability made propoxyphene a drug of choice for right to die societies. It is listed in Dr. Philip Nitschke's The Peaceful Pill Handbook and Dr. Pieter Admiraal's Guide to a Humane Self-Chosen Death.[45][46] "With the withdrawal of the barbiturate sleeping tablets from the medical prescribing list, propoxyphene has become the most common doctor-prescribed medication used by seriously ill people to end their lives."[45] The slang name for the combination of propoxyphene and other drugs used for suicide is "Darvon cocktail".


No comments:
Post a Comment